Table of Contents
This Is Your Endocrine System
BY CONAN MILNER TIME APRIL 30, 2022
Hormones may not seem like a big deal, until they dramatically change. Think about puberty, menopause, pregnancy, or some other moment in life marked by physical, mental, and/or emotional upheaval.
Your body’s endocrine system is the infrastructure responsible for manifesting these life-altering hormonal shifts. However, most of the time, this system is geared toward more routine concerns, like your sleep cycle, tissue repair, and blood sugar stability.
When it comes to our understanding of the endocrine system, most of us have heard of a few glands and a handful of hormones, such as testosterone, estrogen, and cortisol.
What’s not always clear is how everything works together as a whole.
There’s a lot to know about the endocrine system. There are many parts, numerous chemicals, and a relatively recent discovery that explains how the system functions.
Delegating to Glands
The endocrine system consists of about 50 hormones, which are produced by organs called glands. These glands include the pituitary, pineal, thyroid, parathyroid, thymus, pancreas, and adrenals, as well the sex specific glands: testes and ovaries.
Your body has other glands, but only the ones listed above are part of the endocrine system. (The remaining glands, such as sweat glands and tear ducts, belong to what is known as the exocrine system. The lymphatic system also has its own glands.)
Endocrine glands are ductless organs that secrete hormones directly into the bloodstream. You can think of hormones as the communication method glands use to conduct and coordinate bodily functions. Hormones are often called “chemical messengers” because they instruct different parts of the body to perform essential activities at the right moment. Most of this communication happens in the background, without us having to think about it. Just imagine all these chemical messengers sailing through your blood telling different body parts what to do when. They guide our metabolism, reproduction, body temperature, stress response, and much more.
Now add to this rather sophisticated system another system to coordinate it. The endocrine system doesn’t work in isolation. Tiny structures in the brain actually conduct the entire show.
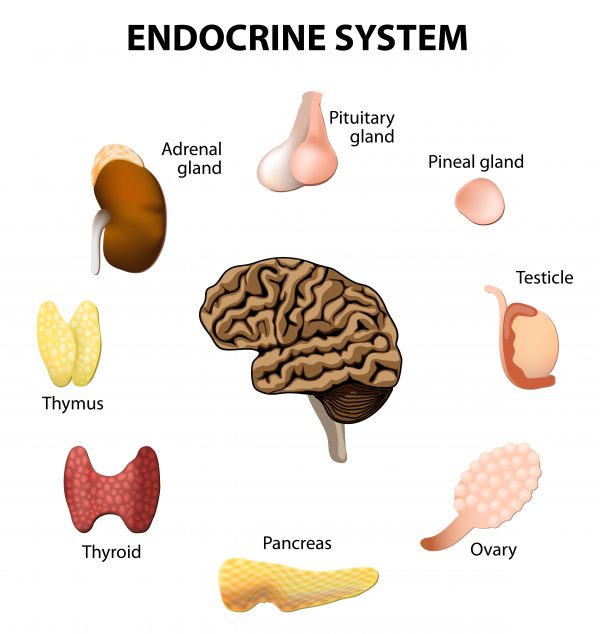
Brain Control
Central command of the endocrine system is something called the HPA axis. H stands for hypothalamus, P for pituitary, and A for adrenal, the gland associated with our fight-or-flight response.
You can think of the HPA axis as the point where your neurological system and endocrine system meet. The pituitary gland, found deep in your brain, is sometimes known as the “master gland” because it controls all the other endocrine glands in the body. Yet it’s only about the size of a pea. This small gland takes its orders from another tiny gland: the hypothalamus, which comes in at about the size of an almond.
The hypothalamus tells the pituitary what to do, and the pituitary sends messages to whichever other gland in the body is specialized for the desired task. For example, the pituitary taps the pancreas to trigger insulin production in order to get nutrients out of the bloodstream and into the cells.
The wild card of the HPA axis is the adrenal glands—three-inch pieces of tissue that rest on the top of each kidney. These are the glands associated with stress and survival, and they produce the stress hormone called cortisol.
The Priority Hormone
The adrenal glands are not found in the brain with the rest of the HPA axis, but when the situation calls for it, these glands become the whole system’s top priority.
For example, when the adrenals secrete a significant amount of cortisol, the body suppresses production of testosterone, a hormone associated with male sex drive and muscle mass.
According to Dr. Andrew Neville, a naturopath in Pennsylvania who specializes in adrenal issues, the body holds back on testosterone in order to focus its immediate resources on survival.
“Your body shuts down the things that aren’t that important, like procreation. It doesn’t really care about your periods or your sex life. … Forget all that. We have to take care of this threat. We can switch that back on after we survive the fight,” Neville said.
Ideally, when the threat passes, normal hormonal function returns. However, chronic stress can delay or even derail this return. If a real or perceived threat is always looming, drawing energy away from functions other than your overactive stress response, the body’s remaining hormonal functions can suffer.
“It all works in this incredibly delicate, dynamic, nuanced response. I tell my patients that when the endocrine system is working, it’s like a professional philharmonic orchestra with a seasoned conductor of 30 years’ experience. It’s exquisite. But if you start to alter that function, then it starts to sound like a middle school band. It’s not that pretty,” Neville said. “There is a lot that can go wrong because hormones really orchestrate much of our physiological mechanisms, such as healing, cellular repair, making neurotransmitters, and turning genes on and off.”
Glandular Duties
With an appreciation for the HPA axis, we can consider the remaining glands of the endocrine system and the jobs they perform.
Let’s start at the top, with the thyroid. This gland is found at the base of the throat, and gets its name from the ancient Greek word for shield. However, some say it looks more like a butterfly. The thyroid oversees a variety of functions—including sleep, metabolism, weight, menstrual cycles, and heart rate.
The thymus gland is associated with immunity. This gland found in the upper chest produces hormones that trigger the release of things like white blood cells and T-cells, but it also secretes hormones to guide your growth. Your thymus is much larger when you’re young, and it starts to shrink when you hit puberty. It becomes progressively smaller as you age, and gradually turns to fat.
The pancreas is the gland associated with digestion. Located next to the stomach, the pancreas is best known for secreting the hormone insulin, but it also produces ghrelin and leptin—hormones broadcast to the HPA axis to communicate our levels of hunger and satiety.
Last, but certainly never least are the sex glands, which, of course, guide reproduction. Testosterone is typically the hormone associated with men, while women are synonymous with estrogen and progesterone. However, both the testes and ovaries each produce all three sex hormones (although in different amounts).
Females develop menstrual cycles that include a regular release of estrogen and progesterone over a 28- to 30-day period that spans from puberty to menopause.
Males have a far more constant release of their primary hormone, testosterone, yet testosterone production still varies on a daily basis. For example, testosterone typically elevates a bit in the morning, drops in the late afternoon, elevates in the evening, only to drop during sleep so it can elevate again in the morning.
Characteristics of Hormones
You might think that, with so much complexity, the discovery of the endocrine system is a rather recent development. But according to Dr. James Giordano, professor of neurology and biochemistry at Georgetown University Medical Center, doctors have understood the basic premise for centuries. He sees a clear precursor to the endocrine system in the ancient concept of bodily humors.
“The whole idea of bodily humors, which was very popular in ancient Greece and ancient Rome, really had something of an intuitive insight into how the endocrine system works,” Giordano said. “These humors had the ability of altering the anatomical capabilities and physiological functions of various systems in the body.”
In the last hundred years or so, our understanding of this elegant system has become much more detailed. We’ve learned, for example, that based on what they’re made of, hormones fall into one of two categories. Those in the steroid group, which includes all the sex and stress hormones, are made of cholesterol. And those in the non-steroid group (everything else) are made of protein.
However, the most revolutionary discovery about the endocrine system has to be the secret behind how hormones actually communicate.
Hormone Receptors
Hormones travel through the bloodstream to deliver their message. But if blood travels everywhere, how does the message only manage to reach the right recipient? Giordano explains that the actual message transfer happens at a molecular level, and hormones only exchange information with tissues that are equipped to read their message.
That’s because hormones can only affect cells that have receptors for that specific hormone. And because cells have many roles, each cell can have receptors for several different hormones.
If the cell has more receptors for a specific hormone, it will be more sensitive to that hormone. Cells with more receptors for a specific hormone are called “up-regulated.” They are tuned to reply to more of that hormone’s signals, perhaps because this is a growth phase in that person’s life or they are going through puberty and so certain genetic traits are activated or turned off.
Hormones can even change what genetic traits are up-regulated or down-regulated in a cell through these receptors.
“The receptor revolution that occurred during the 1970s and 80s was when we really were able to identify the molecular structures that bind to hormones and engage their actions in their various target cells and target systems. This allowed a much more precise understanding of the proverbial lock and key actions that various hormones have on the tissues they affect,” Giordano said.
Hormones are not unique in their lock-and-key communication method. Other biochemical activities outside the endocrine domain also work in a receptor-mediated fashion, such as neurotransmitters in the nervous system, and various components of the immune system.
Subtle Changes, Delicate System
The HPA axis acts as the brains of the whole endocrine process, but the communication works in two ways. After glands receive instructions from central command, they respond with hormonal replies back to the HPA axis. These replies are essential to making the system run more smoothly. The hypothalamus needs feedback to calculate its next move and instruct the pituitary to broadcast a new set of instructions to the glands below. This ongoing endocrine correspondence continues day and night, for as long as we live.
“It is a very delicate, ornate, and articulate set of systems and processes that serve to keep the body in a continuous state of adaptive regulation,” Giordano said.
Much of Giordono’s work explores the role of the mind in the landscape of the endocrine system. He examines the means and processes of hormonal control and its influence on cognition, emotion, and behavior.
“It’s not that we’re biological automatons. We all have primary biological instincts and drives. We’re mammals. But the beauty of the nervous system, whether it’s in a human being, a dog, or a giraffe, is not in its capability for engagement. It’s in the capability of restraint.”
In other words, we all play a conscious role in the ongoing conversation of hormonal communication. Things like puberty and blood sugar regulation may be beyond our conscious control. But other hormonal drives, like sex and hunger, can be a nagging and incessant influence in our lives. However, we ultimately decide how these drives get expressed.
“Our nervous system allows us to be aware of the changes that our body experiences and how they feel, and it certainly allows us to be aware of the consequences of our actions or inaction,” Giordano said.
“Think of it as three interacting domains. We have the sensations of our bodily functions. We have the perceptions and interpretations of what our bodily functions mean. And we have control on how we respond to those bodily sensations.”
The quantities of hormones we produce vary from person to person, and even vary with the same person throughout the day. But if our bodies fail to produce enough of a particular hormone, numerous symptoms can result. Much of the time, treatment for endocrine disorders involves supplementing for hormones we may be deficient in. Think about insulin injections for diabetics, or some other form of hormone replacement therapy.
But there are other ways to improve our endocrine function that don’t require pills or needles.
For example, what we eat and how much food we consume can directly influence the insulin sensitivity of our cells, which means our pancreas doesn’t have to produce so much insulin to get the job done.
Neville says simply trying to live in balance with nature can be a positive influence on hormone levels.
“We are rhythmic beings. We’re designed that way. If a woman can improve her circadian rhythm, she can actually normalize her ovarian hormones. So get up with the sun. Normalize your sleep/wake cycles, and get adequate sleep,” Neville said. “It’s about finding balance. We know this is incredibly important for health in general, but we just have a hard time sticking to it in our modern, toxic, fast-paced, stressful world we live in.”
Managing our stress response can go a long way toward balancing our hormones. Remember, it’s only when the adrenals are not on high alert—flooding our body with cortisol so it is ready to fight or flee—that the rest of our glands are permitted to function at full capacity.
Fortunately, there are things we can do to lower our stress response, such as eating well, meditating, enjoying healthy social engagement, or spending time in nature.
Preventing the body from wasting its precious hormonal resources on chronic stress is important for our overall health.
“We all have thresholds for what we can and can’t tolerate. In some cases these are learned; in many cases, these are trainable and modifiable,” Giordano said.